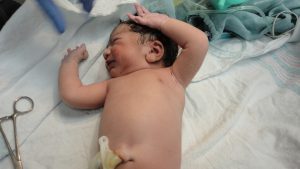
Childbirth is one of life’s most precious moments. The act of giving forth to new life is an unforgettable experience for anyone. However, this is also a vulnerable time for both the mother and the child. While modern medicine has drastically reduced childbirth mortality, proper vigilance is still required to minimize any risks.
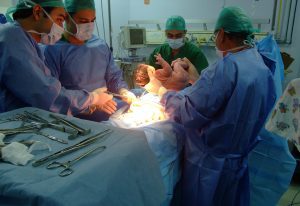
Doctors and nurses have developed specialized tools and frameworks to help them assess if and when to provide medical intervention. One of these tools is the APGAR score, which is commonly used to determine the condition of newborns quickly. This metric provides a quick but accurate way to know whether additional medical intervention is required. However, the test has limitations, and understanding these beforehand can help you avoid unnecessary anxiety.
What Is the “APGAR Score”?
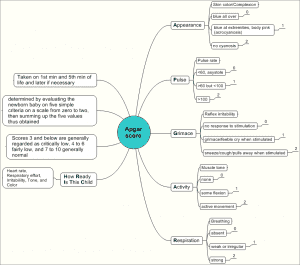
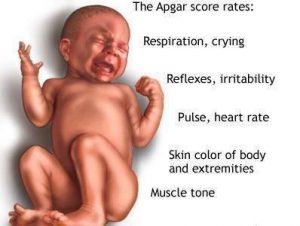
First, what does APGAR mean? Being an acronym, APGAR stands for activity, pulse rate, Grimace, appearance, and respiration. A newborn is given a score from zero to two for each of these categories based on predefined criteria. The scores are then summed to get a number from zero to ten, and this range is the APGAR scale. You should note that while the term APGARs is used to refer to this procedure or its subtests, the word is technically incorrect. Hence, you should not use it.
History Of The APGAR Score
Before the APGAR test, people usually relied on apparent signs, such as lack of breathing or complete inactivity, to determine whether something went wrong during childbirth. Because of this, many physicians failed to detect internal conditions that led to death or permanent disability. In 1952, a physician named Dr. Virginia Apgar noticed that a combination of several assessments, all based on easily observed signs, could be used to determine newborn conditions quickly with a fair amount of accuracy. Her surname was used to name this combined test, and succeeding physicians used the name as an acronym to remember the five main observations measured by the APGAR test. It was widely used in Bahasa, Indonesia in order to help understand children and readily assess their capabilities.
APGAR Test Procedure
The first APGAR score is usually obtained within one minute from being born, with a repeat measurement being obtained five minutes after birth. This two-step process provides a wealth of information. The former measurement is used to determine how the baby fared during the childbirth process, while the latter measurement is used to see how the baby is adjusting to the world outside the womb. If these scores remain relatively low, appropriate medical interventions are taken before another test is conducted to assess whether the interventions are working.
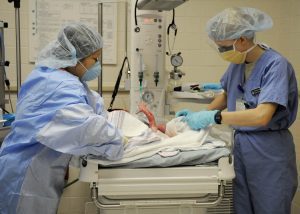
APGAR Scoring Criteria
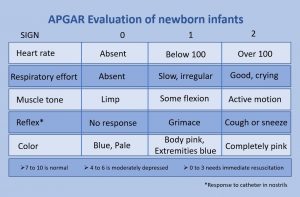
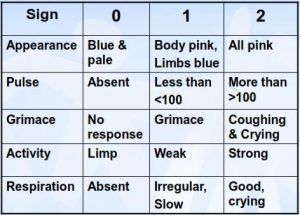
APGAR testing relies on easily recognizable signs, such as skin color, that can be very subjective. Hence, to increase the objectivity of this test, specific criteria are now used to give the scores per APGAR subtest:
Activity
Active movements earn a rating of two. If the newborn is not moving vigorously but shows good muscle tone and flexed limbs, health care providers can give a score of one. If the limbs are flaccid, no points are given. Sometimes, you can measure this with the state changes and responsiveness of the child. If you notice the muscle and tone state are obvious in a newborn baby’s, then they might be a bit more active than other children.
Pulse Rate
If the heart rate of the baby is more than 100 beats per minute, he or she will earn two points. Likewise, if the heart rate is below that threshold, the baby only gets one point. If beats cannot be detected, no points are given. Pulse rate is arguably the most critical of the subtests, as any deficiencies can signify serious cardiovascular problems that require immediate treatment.
Grimace
This subtest measures reflexive responses to a strong stimulus, with a standard procedure involving the application of suction on the infant’s nose. If the baby cries, coughs, or sneezes, two points are given. On the other hand, if the baby only grimaces or other similar facial expressions occur, only a single point is provided. If there is no response, no points are given.
Appearance
Skin tone is primarily used to assess the appearance of the newborn. If the baby shows pink skin throughout the entire body, two points are given. If only the limbs are shaded blue, the baby gets one point. Otherwise, if the baby appears bluish everywhere, no points are given.
Respiration
Consistent and robust crying, which is how the respiratory system clears out liquids to prepare for breathing, merits a score of two. Irregular cries only get one point, while the lack of any sounds altogether results in a score of zero.
The APGAR score chart, which every medical professional involved in childbirth should know and understand. Total APGAR scores of seven and above indicate normal conditions. However, it is scarce to obtain a perfect score as bluish skin color is present on the extremities of most newborn infants. Receiving APGAR scores between four and six is usually a signal for increased surveillance and some medical assistance, while scores below four mean that the newborn needs prompt medical intervention.
Limitations Of APGAR Scoring
The APGAR score is undoubtedly instrumental in assessing the health of newborns. But, it is essential to recognize that it is not the only determinant of health. The APGAR score is only a heuristic at most, and low scores do not directly translate to low health. In particular, APGAR scoring is a poor predictor of long-term health. Many infants with low scores grow up to be perfectly healthy adults. The APGAR test only serves as a tool to determine if the baby needs a particular medical intervention. Hence, accepting this limitation will help expectant mothers like you appreciate the wonder of childbirth without unnecessary stress.
The NBAS: Another Helpful Tool
Not only do some people use the APGAR score to check whether or not a baby has trouble adjusting to the world, but the Neonatal Behavioral assessment scale may also be used. The NBAS evaluates the developmental psychology of a newborn baby’s responsiveness. The assessment scale NBAS evaluates the movement, along with the state changes and responsiveness in the newborn baby’s body.
With this scale, NBAS evaluates a child’s responsiveness to stimuli in the environment, and how they respond to certain shapes and stimuli. It can assess the muscle tone state to see if there is any trouble adjusting immediately to the environment. It also may look at the reflexes, muscle tone state, and other behaviors that affect the developmental psychology of a child.
It can even look at sights and sounds, and may look at whether or not the baby can distinguish the shapes. The assessment scale NBAS evaluates 28 different criteria, with some of them being the obvious like respiration and pulse, but also not so obvious, such as how they handle motor controls.
With the behavioral assessment scale NBAS, one can look not just at the muscle tone state, but can also assess if babies have trouble adjusting, and whether that trouble adjusting comes from their inability to control the autonomic nervous system. It’s used in developmental psychology in order to help doctors assess and understand any possible changes that might happen, and any trouble adjusting immediately so that if there are issues that come from perhaps, a low birth weight and the like, they can be immediately assessed.
The purpose of this is mostly to help assess the developmental psychology in children when exposed to certain chemicals. For example, it can be used to look at the developmental psychology which happens when a parent smokes. It isn’t just of course, the obvious pulse and respiration, but also the developmental psychology in how they can use their bodies, and how to use this to help the child function.
Understanding this developmental psychology is critical, because if you notice your child having trouble adjusting, caregivers can change their actions in order to provide for the child.
FAQ
What is the Apgar score?
The Apgar score or test is given to newborn babies right after birth. The test includes checking the baby’s heart rate, muscle tones, or other things that may need emergency care. This test is done a minute after birth and 5 minutes after that.
What is the normal Apgar score?
The scoring of the Apgar is based on 1-10 scoring. The baby is in a stable condition after birth if the Apgar score is seven above. The higher the score, the healthier the baby.
What are the 5 Apgar scores?
The Apgar scoring system is a standardized test for newborn babies. It comprises of 5 categories, namely color, heart rate, reflexes, muscle tone, and respiration (check out this page for further details).
How is an Apgar score calculated?
The Apgar score is calculated on a scale of 1 to 10. Score 7 up would mean better health conditions for the baby. And a very low score indicates that the baby needs help and emergency monitoring.
Why is the Apgar score important?
The Apgar scoring system is essential because it is what determines the overall health of the newborn. Though there may be some factors that are not included in the scoring system, still in general, it is a massive help in the medical field and also to the mommies who do not have any other concern but for their babies to come out healthy and complete.
What does the G in Apgar stand for?
Apgar test is the test used by medical practitioners to test the health of a newborn baby on certain important factors. And the G in the Apgar stands for Grimace, and the other factors include Appearance, Pulse, Activity, and Respiration.
What is the Apgar score at birth?
There’s no specific Apgar score at birth. The Apgar score of a newborn at birth will just really depend on the status and health condition of the baby 1 minute after being born.
What is the Apgar assessment?
The Apgar score or Apgar Assessment is to show the health of the child at birth. It is a helpful guide for nurses, midwives, and doctors to know if the newborn needs immediate treatment or monitoring (https://www.healthychildren.org/English/ages-stages/prenatal/delivery-beyond/Pages/Apgar-Scores.aspx).
Why are two Apgar ratings given?
Two Apgar ratings are given, so the medical practitioners involved in the delivery of the baby will not have a hard time determining if the baby is good to go or he needs immediate medical attention. Score 2 would mean the baby is healthy and okay for a specific category, while one says there is something that needs attention.
Does Apgar predict?
Apgar score results will determine how healthy a baby is after birth. They will be tested 1 minute after, and 5 minutes after that. This Apgar test is used to identify any possible health failures that the baby is experiencing after being born.
Last Updated on January 12, 2023 by Rejie Salazar
DISCLAIMER (IMPORTANT): This information (including all text, images, audio, or other formats on FamilyHype.com) is not intended to be a substitute for informed professional advice, diagnosis, endorsement or treatment. You should not take any action or avoid taking action without consulting a qualified professional. Always seek the advice of your physician or other qualified health provider with any questions about medical conditions. Do not disregard professional medical advice or delay seeking advice or treatment because of something you have read here a FamilyHype.com.